Streamline Your Business with Pyramos
less claim denials with real-time verification
0
%
more claims processing efficiency
0
%
less administrative costs with automation
0
%
more Eligibility verification Process' Efficiency
0
%
What is Eligibility Verification Tool?
Eligibility Verification Software/Tool is a digital solution designed to streamline the process of verifying patient insurance eligibility for Medicaid, Medicare, and private payers.

Overview of our Eligibility Verification tool
Comprehensive Features for Accurate Medicaid & Medicare Checks
- Daily automated Medicaid and Medicare eligibility checks.
- Nationwide state-certified verifications.
- Confirmation of Medicare coverage.
- Automated notifications for ineligible cases.
- Checks for Medicare Advantage and Traditional Federal Medicare.
- Daily payer eligibility confirmations.
- MCO transfer log with automatic notifications of switches.
- Comprehensive analytics for eligibility and payers.
- Reduces claim denial risks by confirming coverage daily.
- Decreases administrative burden with automated eligibility checks.
- Streamlines workflow, allowing staff to focus on patient care.
- Dedicated customer support for user assistance.
- Comprehensive data security and confidentiality.
- User-friendly interface designed for ease of navigation.
- Automatically checking all participants daily.

Automating Coverage Verification for Better Accuracy and Speed
Efficient Medicaid and Medicare Eligibility Solutions
- Real-Time Verification
- Automated Processes
- Comprehensive Coverage Checks
- User-Friendly Interface
- Integration with EHR Systems
- Alerts and Notifications
- Reporting and Analytics

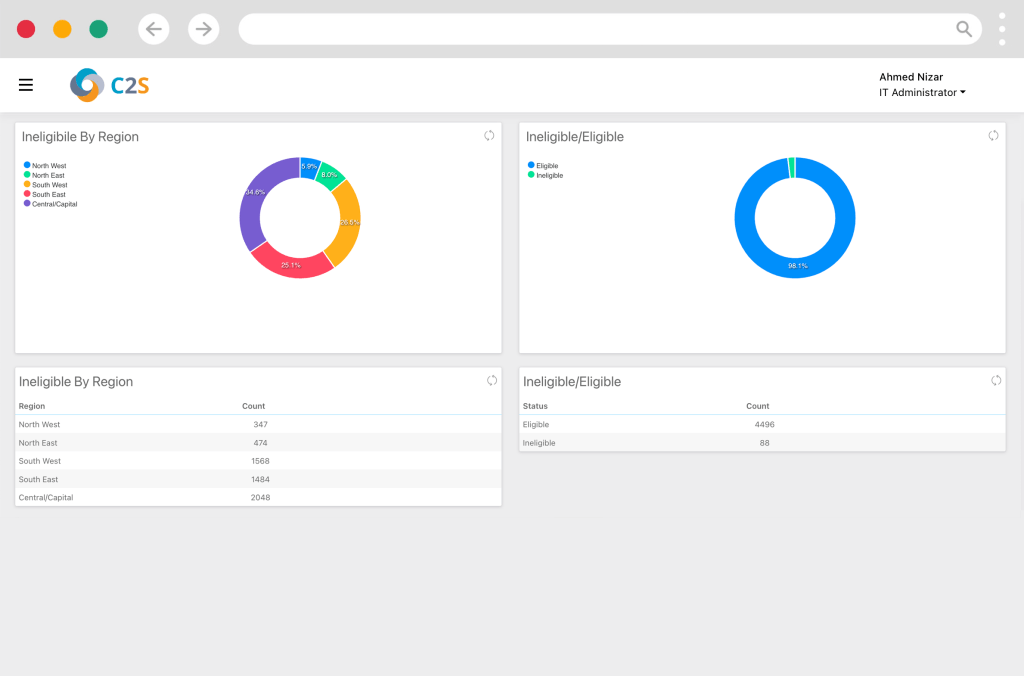
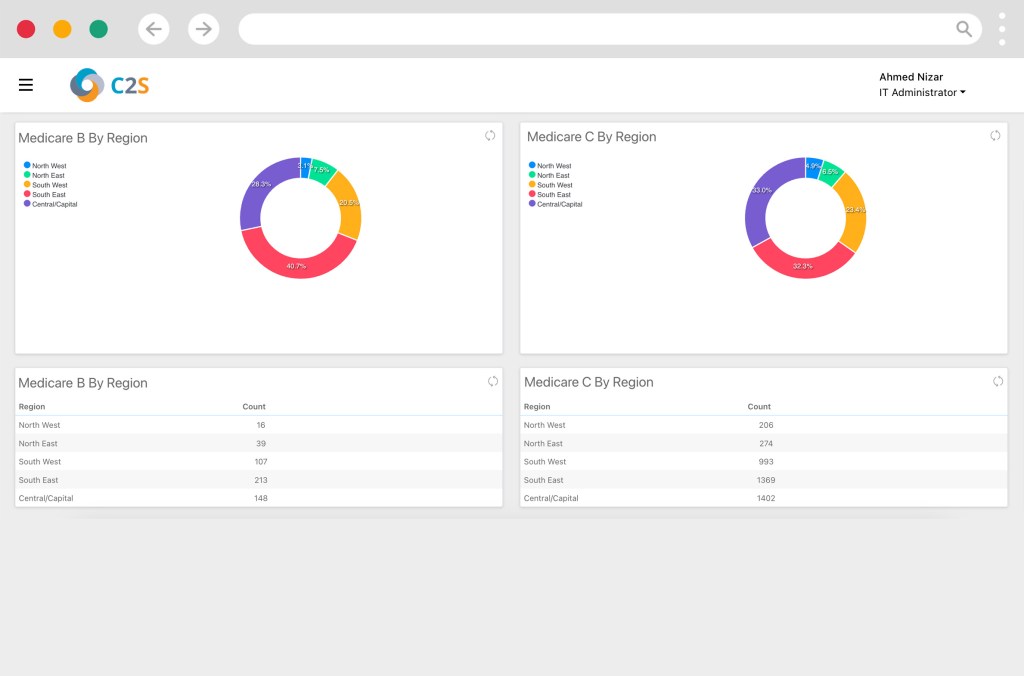
Customized Verification Services for Healthcare, Insurance
Empowering a Range of Industries with Tailored Eligibility Solutions
Learn More ↗
Behavioral Health
Learn More ↗
Assistive Technology
Learn More ↗
Long-Term Support (LTSS)